Back
Wound Care
064 - The WET Study: Wound care, Education, and Talking. How better communication can heal wounds

Justin Ady, MD – Faculty, Vascular Surgery, Rutgers Robert Wood Johnson University Hospital; Saum Rahimi, MD – Division Chief, Vascular Surgery, Rutgers Robert Wood Johnson University Hospital
Purpose: Wet-to-dry dressings are a form of wound treatment that is economical, absorptive, and permeable to gasses while providing mechanical debridement to infected wounds, as well as those that require frequent changes. Saline-moistened woven gauze dressings are frequently used in vascular surgery, oftentimes being changed by both the surgical team and nursing staff. Due to the wide range of nursing experience, post-surgical care education, and complexity of wound care orders placed by the vascular surgery department, a quality improvement initiative was developed to improve upon all of these variables.
Material and Methods: The nursing staff from the vascular surgery ward were anonymously surveyed during change of shift utilizing a multiple-choice quiz to assess their understanding of wet-to-dry dressings, as well as proper dressing change techniques. After recording the results, a 10-minute in-service educational meeting was performed at the nurse’s station, with demonstrations on properly performing dressing changes. After the demonstration, the same initial survey was administered to assess their new level of understanding, which was recorded and compared to the pre-survey results.
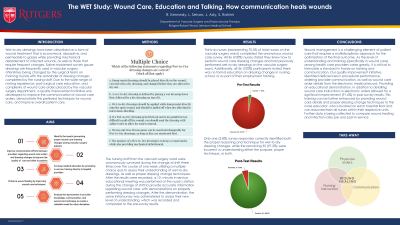
Results: Thirty-six nurses (~70.5% of total nurses on the vascular surgery ward) completed the anonymous wound care survey. All 36 (100%) nurses stated they knew how to perform wound care dressing changes and had previously performed wet-to-dry dressings on the vascular surgery ward. Additionally, all 36 (100%) participants stated there was no formal education on dressing changes in nursing school, or as part of their employment training. Only one (2.8%) survey responder correctly identified both the proper reasoning and technique for wet-to-dry dressing changes, while the remaining 35 (97.2%) were incorrect in understanding either the purpose, proper technique or both. Post-survey results demonstrated an overall improvement of 91.6%, where 34 out of 36 (~94.4%) responders correctly identified both the purpose and proper technique of the wet-to-dry dressing.
Conclusions: Our quality improvement initiative identified deficiencies in procedural performance, provider communication, as well as order details within the electronic medical record. Providing an educational demonstration, in addition to detailing wound care instructions in electronic orders allowed for a significant improvement (91.6%) in post-survey results.
Material and Methods: The nursing staff from the vascular surgery ward were anonymously surveyed during change of shift utilizing a multiple-choice quiz to assess their understanding of wet-to-dry dressings, as well as proper dressing change techniques. After recording the results, a 10-minute in-service educational meeting was performed at the nurse’s station, with demonstrations on properly performing dressing changes. After the demonstration, the same initial survey was administered to assess their new level of understanding, which was recorded and compared to the pre-survey results.
Results: Thirty-six nurses (~70.5% of total nurses on the vascular surgery ward) completed the anonymous wound care survey. All 36 (100%) nurses stated they knew how to perform wound care dressing changes and had previously performed wet-to-dry dressings on the vascular surgery ward. Additionally, all 36 (100%) participants stated there was no formal education on dressing changes in nursing school, or as part of their employment training. Only one (2.8%) survey responder correctly identified both the proper reasoning and technique for wet-to-dry dressing changes, while the remaining 35 (97.2%) were incorrect in understanding either the purpose, proper technique or both. Post-survey results demonstrated an overall improvement of 91.6%, where 34 out of 36 (~94.4%) responders correctly identified both the purpose and proper technique of the wet-to-dry dressing.
Conclusions: Our quality improvement initiative identified deficiencies in procedural performance, provider communication, as well as order details within the electronic medical record. Providing an educational demonstration, in addition to detailing wound care instructions in electronic orders allowed for a significant improvement (91.6%) in post-survey results.
