Back
Aneurysm/Dissection
127 - Covered Stent Placement for Gastroduodenal Artery Stump Pseudoaneurysm Rupture Following Selective Coil Embolization

Eric Schoen, BA – Medical Student, University of Louisville; Nana Ohene-Baah, MD – Assistant Professor, Interventional Radiology, University of Louisville
Purpose: The gastroduodenal artery (GDA) stump pseudoaneurysm is a common site of delayed massive hemorrhage following pancreaticoduodenectomy. We present a case of a GDA stump pseudoaneurysm rupture and coil unraveling after a selective coil embolization successfully managed with placement of a covered stent across the common and proper hepatic arteries.
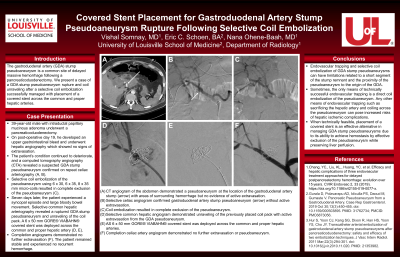
Material and Methods: A 39-year-old male with an intraductal papillary mucinous adenoma of the pancreas underwent a pancreaticoduodenectomy. Nineteen days after the operation, he developed an upper gastrointestinal bleed and underwent hepatic angiography which showed no signs of extravasation. The patient’s condition continued to deteriorate, and a computed tomography angiography (CTA) revealed a suspected GDA stump pseudoaneurysm confirmed on repeat celiac arteriography. Selective coil embolization of the pseudoaneurysm using 6 x 30, 6 x 35, 8 x 35 mm microcoils resulted in complete exclusion of the pseudoaneurysm. Seven days later, the patient experienced a syncopal episode and large bloody bowel movement. Selective common hepatic arteriography revealed a ruptured GDA stump pseudoaneurysm and unraveling of the coil pack. Subsequently, a 6 x 50 mm covered stent was deployed across the common and proper hepatic artery. Completion angiograms were performed which demonstrated no further extravasation. The patient remained stable and experienced no recurrent hemorrhage.
Results: Endovascular trapping and selective coil embolization of GDA stump pseudoaneurysms can have limitations related to a short segment of the stump remnant and the proximity of the pseudoaneurysm to the origin of the GDA. Sometimes, the only means of technically successful endovascular trapping is a direct coil embolization of the pseudoaneurysm. Any other means of endovascular trapping such as sacrificing the hepatic artery and coiling across the pseudoaneurysm can pose increased risks of hepatic ischemic complications. When technically feasible, placement of a covered stent is an effective alternative in managing GDA stump pseudoaneurysms.
Conclusions: Covered stent placement is a viable alternative in managing hemorrhage from GDA stump pseudoaneurysms due to its ability to achieve hemostasis by effective exclusion of the pseudoaneurysm while preserving liver perfusion.
Material and Methods: A 39-year-old male with an intraductal papillary mucinous adenoma of the pancreas underwent a pancreaticoduodenectomy. Nineteen days after the operation, he developed an upper gastrointestinal bleed and underwent hepatic angiography which showed no signs of extravasation. The patient’s condition continued to deteriorate, and a computed tomography angiography (CTA) revealed a suspected GDA stump pseudoaneurysm confirmed on repeat celiac arteriography. Selective coil embolization of the pseudoaneurysm using 6 x 30, 6 x 35, 8 x 35 mm microcoils resulted in complete exclusion of the pseudoaneurysm. Seven days later, the patient experienced a syncopal episode and large bloody bowel movement. Selective common hepatic arteriography revealed a ruptured GDA stump pseudoaneurysm and unraveling of the coil pack. Subsequently, a 6 x 50 mm covered stent was deployed across the common and proper hepatic artery. Completion angiograms were performed which demonstrated no further extravasation. The patient remained stable and experienced no recurrent hemorrhage.
Results: Endovascular trapping and selective coil embolization of GDA stump pseudoaneurysms can have limitations related to a short segment of the stump remnant and the proximity of the pseudoaneurysm to the origin of the GDA. Sometimes, the only means of technically successful endovascular trapping is a direct coil embolization of the pseudoaneurysm. Any other means of endovascular trapping such as sacrificing the hepatic artery and coiling across the pseudoaneurysm can pose increased risks of hepatic ischemic complications. When technically feasible, placement of a covered stent is an effective alternative in managing GDA stump pseudoaneurysms.
Conclusions: Covered stent placement is a viable alternative in managing hemorrhage from GDA stump pseudoaneurysms due to its ability to achieve hemostasis by effective exclusion of the pseudoaneurysm while preserving liver perfusion.
