Back
PAD: Other
109 - Enhancing Survival and Patency of Saphenous Vein Grafts using a Xenograft Model

Christopher Frontario, DO – Vascular Fellow, Vascular Surgery, Englewood Health Medical Center; Thomas Hoffman, BS – Associate Director, Surgical Sciences Research Laboratory, Englewood Health Medical Center; Brendan Hammond, BS – Research Intern, Surgical Sciences Research Laboratory, Englewood Health Medical Center; Saahil Patel, BS – Research Intern, Surgical Sciences Research Laboratory, Englewood Health Medical Center; Robert Pergolizzi, PhD – Director, Surgical Sciences Research Laboratory, Englewood Health Medical Center; Thomas Bernik, MD – Chairman of the Department of Vascular Surgery, Vascular Surgery, Englewood Health Medical Center
Purpose: The saphenous vein graft (SVG) has been the conduit of choice for over 50 years, but its lack of availability makes its superior utility unreliable. Because of the paucity of autologous vein grafts and poor results of alternative bypass conduits, we hypothesized vein allografts can be used for patients with limb-threatening ischemia who do not have adequate vein conduit for restorative bypass surgery. Despite improvements in outcomes in the past decade, graft patency and conduit availability remain the ‘Achilles’ heel’ of this procedure.
Remodeling processes of the vein graft start within days after harvesting and grafting, leading to the formation of intimal hyperplasia; the primary cause of intermediate-phase vein graft stenosis and occlusion. Even autologous saphenous vein grafts are affected, leading to poor long-term patency, with handling and preimplantation treatment having an impact on mean time to failure.
Material and Methods: To study the question of how to treat vessels for implantation such that they are less “visible” to the immune system, we have developed an IRB/IACUC-approved model in which human saphenous vein segments are grafted into rats via infra-renal inter-positional aorta grafts, after subjecting the veins to various treatments intended to extend patency. This xenograft model accelerates the rate of failure due to the extreme difference in species biomarkers. We have performed SVGs on 47 Sprague-Dawley rats, using either no pretreatment, or one of several pretreatment cocktails including various fixatives, decellularizing agents, nucleases, proteases and alcohols, at varying concentrations for periods of time from 1 to 9 months.
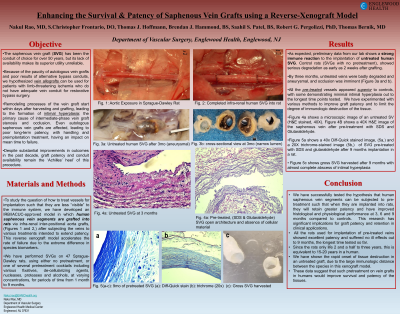
Results: Preliminary data from our lab shows a strong immune reaction to the implantation of human SVG, as expected. Control rats (SVGs with no pretreatment), show serious degradation as early as 2 weeks after grafting. All the pretreated vessels appeared superior to controls, with some demonstrating minimal intimal hyperplasia out to the longest time points tested.
Conclusions: We have successfully tested the hypothesis that human saphenous vein segments can be subjected to pre-treatment such that when they are implanted into rats, they will retain greater patency and have improved histological and physiological performance at 3, 6 and 9 months compared to controls. This research has significant implications for graft patency and retention in clinical applications.
Remodeling processes of the vein graft start within days after harvesting and grafting, leading to the formation of intimal hyperplasia; the primary cause of intermediate-phase vein graft stenosis and occlusion. Even autologous saphenous vein grafts are affected, leading to poor long-term patency, with handling and preimplantation treatment having an impact on mean time to failure.
Material and Methods: To study the question of how to treat vessels for implantation such that they are less “visible” to the immune system, we have developed an IRB/IACUC-approved model in which human saphenous vein segments are grafted into rats via infra-renal inter-positional aorta grafts, after subjecting the veins to various treatments intended to extend patency. This xenograft model accelerates the rate of failure due to the extreme difference in species biomarkers. We have performed SVGs on 47 Sprague-Dawley rats, using either no pretreatment, or one of several pretreatment cocktails including various fixatives, decellularizing agents, nucleases, proteases and alcohols, at varying concentrations for periods of time from 1 to 9 months.
Results: Preliminary data from our lab shows a strong immune reaction to the implantation of human SVG, as expected. Control rats (SVGs with no pretreatment), show serious degradation as early as 2 weeks after grafting. All the pretreated vessels appeared superior to controls, with some demonstrating minimal intimal hyperplasia out to the longest time points tested.
Conclusions: We have successfully tested the hypothesis that human saphenous vein segments can be subjected to pre-treatment such that when they are implanted into rats, they will retain greater patency and have improved histological and physiological performance at 3, 6 and 9 months compared to controls. This research has significant implications for graft patency and retention in clinical applications.
