Back
PAD: SFA Intervention
098 - BEnefit of LONGitudinal Micro-Incisions Prior to Paclitaxel Coated Balloon Angioplasty (BELONG Study) : 12-month Results

Jean-Baptiste Dexpert, MD – Angiology, HFR Fribourg, Hôpital Cantonal; Rolf Engelberger, MD – Angiology, HFR Fribourg, Hôpital Cantonal; Daniel Hayoz, MD – Angiology, HFR Fribourg, Hôpital Cantonal; Eric Secemsky, MD, MSc, RPVI, FACC, FAHA, FSCAI, FSVM – Assistant Professor of Medicine, Beth Israel Deaconess Medical Center, Harvard Medical School
Purpose: The Use of FLEX Vessel Prep™ System (FLEX VPTM) before drug coated balloon (DCB) angioplasty may improve acute and long-term clinical outcomes. FLEX VP is a novel, intuitive device with a dual mechanism of action (MOA) that modifies the plaque by creating longitudinal, controlled-depth micro-incisions, preparing the vessel for final therapy. The purpose of this study was to assess the 12-month outcomes of subjects who underwent FLEX vessel preparation prior to DCB.
Material and Methods: Subjects with symptomatic lower extremity peripheral artery disease and a Rutherford Class of 2-5 with 70% or more de novo, restenotic, or in-stent stenosis of the superficial femoral or popliteal arteries were included. Subjects with recent thrombosis, risk of distal embolization, or extremely calcified lesions (>270° of the artery circumference over >15 cm), and previous DCB use within 15 months were excluded. During the procedure, three to four passes with FLEX VP were performed at the operator’s discretion prior to DCB. Provisional stenting was utilized in cases of residual stenosis > 50% post-DCB.
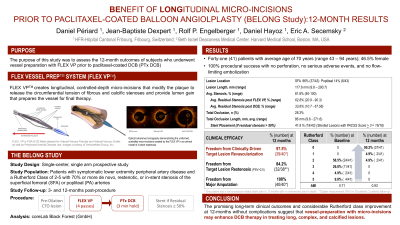
Results: There were 41 subjects treated in this study with an average lesion length of 187 mm (20-430), average stenosis of 89%, and an occlusion rate of 32% with a CTO length of 124 mm. 80% of the lesions had calcification and 30% exhibiting severe calcification. Severe dissections after FLEX VP and DCB (NHLBI Grade D-F) occurred in 10% of cases. Stenting was utilized in 39% of cases.
The freedom from target lesion revascularization (TLR) was 97.6% at 12 months. 42% of the lesions were at a Rutherford class of 3 or higher at baseline. At 12 months, 95% of the lesions were at a Rutherford class 1 or lower (with no lesions greater than Rutherford class of 2). There were no amputations at 12-months.
Conclusions: Treating long, complex, and calcified lesions with FLEX VP prior to DCB provides substantial clinical benefit. The promising long-term outcomes of 97.6% freedom from TLR, low severe dissection rate, and considerable Rutherford class improvement at 12-months, suggest micro-incisions enhances DCB therapy.
Material and Methods: Subjects with symptomatic lower extremity peripheral artery disease and a Rutherford Class of 2-5 with 70% or more de novo, restenotic, or in-stent stenosis of the superficial femoral or popliteal arteries were included. Subjects with recent thrombosis, risk of distal embolization, or extremely calcified lesions (>270° of the artery circumference over >15 cm), and previous DCB use within 15 months were excluded. During the procedure, three to four passes with FLEX VP were performed at the operator’s discretion prior to DCB. Provisional stenting was utilized in cases of residual stenosis > 50% post-DCB.
Results: There were 41 subjects treated in this study with an average lesion length of 187 mm (20-430), average stenosis of 89%, and an occlusion rate of 32% with a CTO length of 124 mm. 80% of the lesions had calcification and 30% exhibiting severe calcification. Severe dissections after FLEX VP and DCB (NHLBI Grade D-F) occurred in 10% of cases. Stenting was utilized in 39% of cases.
The freedom from target lesion revascularization (TLR) was 97.6% at 12 months. 42% of the lesions were at a Rutherford class of 3 or higher at baseline. At 12 months, 95% of the lesions were at a Rutherford class 1 or lower (with no lesions greater than Rutherford class of 2). There were no amputations at 12-months.
Conclusions: Treating long, complex, and calcified lesions with FLEX VP prior to DCB provides substantial clinical benefit. The promising long-term outcomes of 97.6% freedom from TLR, low severe dissection rate, and considerable Rutherford class improvement at 12-months, suggest micro-incisions enhances DCB therapy.
