Back
Venous Intervention
070 - Liver transplant portal vein stenosis - Long term follow up of angioplasty and stent placement

Gerard Healy, MBBCh, FFRRCSI, PhD – Vascular, interventional and abdominal radiologist, Radiology, St Vincent’s University Hospital, Dublin, Ireland; Kong Teng Tan, MD, FRCR, FRCPC – Vascular and Interventional Radiologist, Interventional Radiology, University of Toronto
Purpose: To investigate patency of percutaneous transhepatic angioplasty and/or stenting of portal vein (PV) stenosis in adult liver transplant (LT) recipients.
ABBREVIATIONS: LT = liver transplant, PV = portal vein, PVS = portal vein stenosis, LDLT = living donor liver transplantation, DDLT = deceased donor liver transplant
Material and Methods: A single-institution, retrospective study of patients treated between December 2000 to September 2021. From a total of 3387 deceased donor and living donor liver adult transplant (2533 DDLT and 854 LDLT) recipients, 13 were treated for clinically significant portal vein stenosis (PVS) with percutaneous transhepatic angioplasty and/or stenting. The primary endpoint was primary patency, compared between groups. Secondary endpoints included time to first intervention, time to recurrent stenosis, technical success, clinical success, and complications.
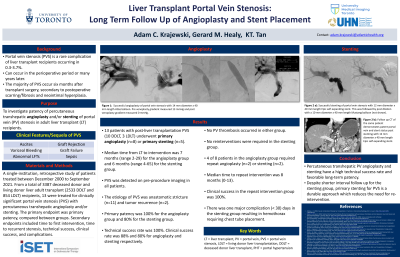
Results: 13 patients with post-liver transplantation PVS (10 DDLT, 3 LDLT) underwent angioplasty (n=8) or stenting (n=5). Median time from LT to intervention was 7 months (range 2-29) for the angioplasty group and 6 months (range 4-65) for the stenting group. PVS was detected on pre-procedure imaging in all patients. The etiology of PVS was anastomotic stricture (n=11) and tumor recurrence (n=2). Primary patency was 100% for the angioplasty group and 80% for the stenting group. Technical success rate was 100%. Clinical success rate was 88% and 80% for angioplasty and stenting respectively. No PV thrombosis occurred in either group. No reinterventions were required in the stenting group. 4 of 8 patients in the angioplasty group required repeat angioplasty (n=2) or stenting (n=2). Median time to repeat intervention was 8 months (0-13). Clinical success in the repeat intervention group was 100%. There was one major complication ( < 30) days in the stenting group resulting in hemothorax requiring chest tube placement.
Conclusions: Percutaneous transhepatic PV angioplasty and stenting have a high technical success rate and favorable long-term patency. Despite shorter interval follow up for the stenting group, this group required no repeat interventions.
ABBREVIATIONS: LT = liver transplant, PV = portal vein, PVS = portal vein stenosis, LDLT = living donor liver transplantation, DDLT = deceased donor liver transplant
Material and Methods: A single-institution, retrospective study of patients treated between December 2000 to September 2021. From a total of 3387 deceased donor and living donor liver adult transplant (2533 DDLT and 854 LDLT) recipients, 13 were treated for clinically significant portal vein stenosis (PVS) with percutaneous transhepatic angioplasty and/or stenting. The primary endpoint was primary patency, compared between groups. Secondary endpoints included time to first intervention, time to recurrent stenosis, technical success, clinical success, and complications.
Results: 13 patients with post-liver transplantation PVS (10 DDLT, 3 LDLT) underwent angioplasty (n=8) or stenting (n=5). Median time from LT to intervention was 7 months (range 2-29) for the angioplasty group and 6 months (range 4-65) for the stenting group. PVS was detected on pre-procedure imaging in all patients. The etiology of PVS was anastomotic stricture (n=11) and tumor recurrence (n=2). Primary patency was 100% for the angioplasty group and 80% for the stenting group. Technical success rate was 100%. Clinical success rate was 88% and 80% for angioplasty and stenting respectively. No PV thrombosis occurred in either group. No reinterventions were required in the stenting group. 4 of 8 patients in the angioplasty group required repeat angioplasty (n=2) or stenting (n=2). Median time to repeat intervention was 8 months (0-13). Clinical success in the repeat intervention group was 100%. There was one major complication ( < 30) days in the stenting group resulting in hemothorax requiring chest tube placement.
Conclusions: Percutaneous transhepatic PV angioplasty and stenting have a high technical success rate and favorable long-term patency. Despite shorter interval follow up for the stenting group, this group required no repeat interventions.
