Back
Visceral Intervention
100 - Treatment of Pancreatitis Associated Visceral Arterial Pseudoaneurysms

Omair Ali, BS – Medical Student, University of Illinois College of Medicine; Raj Kakarla, MD – Associate Medical Director, Department of Radiology, Javon Bea Hospital–Riverside
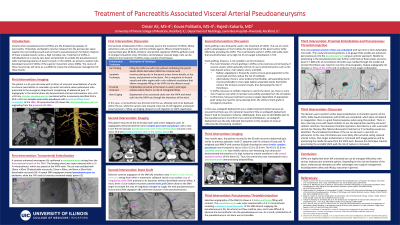
Purpose: Visceral artery pseudoaneurysms (VAPAs) are life-threatening sequelae of pancreatitis. Proteolytic and lipolytic enzymes released into the perivascular space weaken the surrounding vessels and can lead to pseudoaneurysm formation. Rupture of these unstable lesions carries a high mortality rate. Although treatment of VAPAs is individualized on a case-by-case basis, all approaches attempt to exclude the pseudoaneurysm while maintaining patency of parent vessels. This exhibit will provide a review of the endovascular management of these lesions with the help of a case study outlining the clinical course of a patient with recurrent VAPAs.
Material and Methods: A retrospective electronic medical record review was performed to analyze the case of a 51 year old male who underwent three consecutive interventions for recurrent superior mesenteric artery (SMA) pseudoaneurysms in the background of chronic pancreatitis and a hemorrhagic pseudocyst.
Results: The patient presented with a VAPA supplied by a small feeding vessel in a proximal branch of the SMA during an acute episode of pancreatitis. Embolization of the feeding vessel with several detachable micro-coils led to total exclusion of flow from the pseudoaneurysm. Two weeks later, the patient presented with symptoms of pancreatitis and an SMA arteriogram revealed a new delayed ovoid contrast collection arising from an area of irregularity of the SMA proximal to its branches without a defined arterial in-flow to the pseudoaneurysm. With no clear neck to embolize, this lesion was treated via the deployment of a short balloon-mounted covered stent that successfully excluded the segment of the SMA supplying the pseudoaneurysm. Several weeks later, another VAPA was identified arising from a small branch of the SMA. However, this lesion demonstrated no arterial out-flow past the pseudoaneurysm. Using a microcatheter, two micro-coils were deployed within the feeding vessel, thus achieving successful flow-exclusion. Additionally, percutaneous thrombin injection was used to embolize the pseudoaneurysm cavity under ultrasound, fluoroscopic, and CT guidance.
Conclusions: VAPAs are highly fatal when left untreated, but can be managed effectively with various endovascular treatment options. Depending on the size and location of the lesion, endovascular therapies can offer advantages over surgical management, including better safety and efficacy outcomes in general.
Material and Methods: A retrospective electronic medical record review was performed to analyze the case of a 51 year old male who underwent three consecutive interventions for recurrent superior mesenteric artery (SMA) pseudoaneurysms in the background of chronic pancreatitis and a hemorrhagic pseudocyst.
Results: The patient presented with a VAPA supplied by a small feeding vessel in a proximal branch of the SMA during an acute episode of pancreatitis. Embolization of the feeding vessel with several detachable micro-coils led to total exclusion of flow from the pseudoaneurysm. Two weeks later, the patient presented with symptoms of pancreatitis and an SMA arteriogram revealed a new delayed ovoid contrast collection arising from an area of irregularity of the SMA proximal to its branches without a defined arterial in-flow to the pseudoaneurysm. With no clear neck to embolize, this lesion was treated via the deployment of a short balloon-mounted covered stent that successfully excluded the segment of the SMA supplying the pseudoaneurysm. Several weeks later, another VAPA was identified arising from a small branch of the SMA. However, this lesion demonstrated no arterial out-flow past the pseudoaneurysm. Using a microcatheter, two micro-coils were deployed within the feeding vessel, thus achieving successful flow-exclusion. Additionally, percutaneous thrombin injection was used to embolize the pseudoaneurysm cavity under ultrasound, fluoroscopic, and CT guidance.
Conclusions: VAPAs are highly fatal when left untreated, but can be managed effectively with various endovascular treatment options. Depending on the size and location of the lesion, endovascular therapies can offer advantages over surgical management, including better safety and efficacy outcomes in general.
