Back
Visceral Intervention
125 - Endovascular Shunt Creation for Chronic Portomesenteric Thrombosis: A Retrospective Analysis of Safety and Efficacy

Daryl Goldman, MD – Resident Physician, Diagnostic, Molecular, and Interventional Radiology, Mount Sinai Hospital; Rahul Patel, MD – Assistant Professor, Diagnostic, Molecular, and Interventional Radiology, Mount Sinai Hospital
Purpose: To assess safety and efficacy of endovascular shunt creation for chronic portomesenteric thrombosis (PMT) in patients who are refractory to standard-of-care therapy at a single tertiary care center.
Material and Methods: Chronic PMT patients evaluated by a multidisciplinary team of IR, liver medicine, and transplant surgery who underwent endovascular shunt placement between July 1, 2013 and November 15th, 2021 were identified. Baseline and follow-up laboratory, clinical and radiographic reports and images were reviewed. Primary outcomes included primary shunt patency and adverse events. Secondary outcomes were technical success, symptom resolution and mortality. Kaplan-Meier survival analysis was used to assess primary shunt patency and overall shunt patency (including secondary shunt re-interventions).
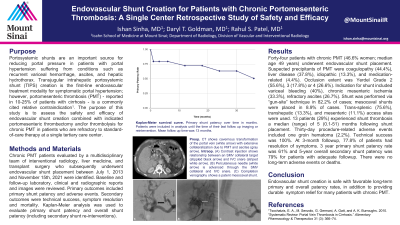
Results: Forty-four patients with chronic PMT (46.6% woman; median age, 48.5 years) underwent endovascular shunt placement. Suspected precipitants of PMT were coagulopathy (44.4%), liver disease (37.8%), idiopathic (13.3%), and medication-related (4.4%). Occlusion extent was Yerdel Grade 2 (55.6%), 3 (17.8%) or 4 (26.6%). Indication for shunt included variceal bleeding (40%), chronic mesenteric ischemia (33.3%), refractory ascites (26.7%). Shunt was performed via “gun-site technique” in 82.2% of cases and mesocaval shunts were placed in 8.9% of cases. Trans-splenic (75.6%), transhepatic (13.3%), and mesenteric (11.1%) access sites were used. At 3 years, freedom from primary shunt thrombosis was 61%, and overall shunt patency at 5 years following secondary interventions was 79%. Thirteen patients (29%) experienced shunt thrombosis a median (range) of 5 (0.1-51) months following shunt placement. Thirty-day procedure-related adverse events included 1 groin hematoma (2.2%). Technical success was 100%. At 3 months follow-up, 77.8% of patients had resolution of symptoms. There were no significant long-term adverse events or deaths.
Conclusions: Endovascular shunt creation is safe with long-term primary and overall patency and can provide symptom relief for the majority of patients with chronic PMT.
Material and Methods: Chronic PMT patients evaluated by a multidisciplinary team of IR, liver medicine, and transplant surgery who underwent endovascular shunt placement between July 1, 2013 and November 15th, 2021 were identified. Baseline and follow-up laboratory, clinical and radiographic reports and images were reviewed. Primary outcomes included primary shunt patency and adverse events. Secondary outcomes were technical success, symptom resolution and mortality. Kaplan-Meier survival analysis was used to assess primary shunt patency and overall shunt patency (including secondary shunt re-interventions).
Results: Forty-four patients with chronic PMT (46.6% woman; median age, 48.5 years) underwent endovascular shunt placement. Suspected precipitants of PMT were coagulopathy (44.4%), liver disease (37.8%), idiopathic (13.3%), and medication-related (4.4%). Occlusion extent was Yerdel Grade 2 (55.6%), 3 (17.8%) or 4 (26.6%). Indication for shunt included variceal bleeding (40%), chronic mesenteric ischemia (33.3%), refractory ascites (26.7%). Shunt was performed via “gun-site technique” in 82.2% of cases and mesocaval shunts were placed in 8.9% of cases. Trans-splenic (75.6%), transhepatic (13.3%), and mesenteric (11.1%) access sites were used. At 3 years, freedom from primary shunt thrombosis was 61%, and overall shunt patency at 5 years following secondary interventions was 79%. Thirteen patients (29%) experienced shunt thrombosis a median (range) of 5 (0.1-51) months following shunt placement. Thirty-day procedure-related adverse events included 1 groin hematoma (2.2%). Technical success was 100%. At 3 months follow-up, 77.8% of patients had resolution of symptoms. There were no significant long-term adverse events or deaths.
Conclusions: Endovascular shunt creation is safe with long-term primary and overall patency and can provide symptom relief for the majority of patients with chronic PMT.
