Back
Visceral Intervention
141 - Comparison of Role of Angiography for Penetrating to Blunt Trauma Using a National Trauma Databank

Mikin Patel, MD – Assistant Professor, Radiology, University of Chicago; Nima Kokabi, MD – Assistant Professor, Radiology, Emory University School of Medicine; Osman Ahmed, MD – Assistant Professor, Radiology, University of Chicago
Purpose: To understand the effect of interventional radiology (IR) treatment among patients with penetrating (PT) compared to those with blunt abdominal trauma (BT) who received blood transfusion within the first 4 hours of arrival undergoing emergent angiography in the national trauma databank (NTDB)
Material and Methods: The National Trauma Databank was queried from 2013 to 2019 for patients who received packed RBCs or whole blood within first 4 hours after arrival. Using the Abbreviated Injury Scale (AIS) pre-dot codes, patients with trauma to the abdomen, extremities, and thorax were included. Patients with trauma to the head, spine, or whole body were excluded. Patients who received IR intervention (including angiography, angioembolization, and stenting) for PT and BT were identified. Kaplan-Meier survival curves were created to visualize mortality rate based on LOS. Multivariable Cox proportional hazard regression with marginal effects, adjusted for comorbidities and injury severity, was conducted to assess the effect of IR intervention for PT compared to BT.
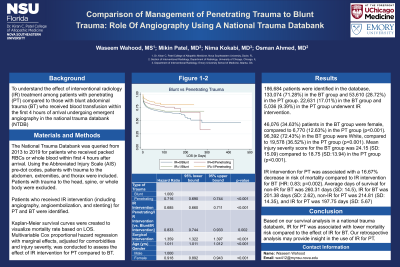
Results: 186,684 patients were identified in the database, 133,074 (71.28%) in the BT group and 53,610 (28.72%) in the PT group. 22,631 (17.01%) in the BT group and 5,036 (9.39%) in the PT group underwent IR intervention. 46,076 (34.63%) patients in the BT group were female, compared to 6,770 (12.63%) in the PT group (p < 0.001). 96,392 (72.43%) in the BT group were White, compared to 19,578 (36.52%) in the PT group (p < 0.001). Mean injury severity score (ISS) for the BT group was 24.15 (SD: 15.09) compared to 18.75 (SD:13.94) in the PT group (p < 0.001).
IR intervention for PT was associated with a 16.67% decrease in risk of mortality compared to IR intervention for BT (HR: 0.83; 95% CI: 0.74-0.93; p=0.002). Average days of survival for non-IR for BT was 260.31 days (SD: 14.5), IR for BT was 201.38 days (SD: 2.62), non-IR for PT was 214.81 (SD: 14.35), and IR for PT was 197.75 days (SD: 5.67)
Conclusions: Based on our survival analysis in a national trauma databank, IR for PT was associated with lower mortality risk compared to the effect of IR for BT. Our retrospective analysis may provide insight in the use of IR for PT.
Material and Methods: The National Trauma Databank was queried from 2013 to 2019 for patients who received packed RBCs or whole blood within first 4 hours after arrival. Using the Abbreviated Injury Scale (AIS) pre-dot codes, patients with trauma to the abdomen, extremities, and thorax were included. Patients with trauma to the head, spine, or whole body were excluded. Patients who received IR intervention (including angiography, angioembolization, and stenting) for PT and BT were identified. Kaplan-Meier survival curves were created to visualize mortality rate based on LOS. Multivariable Cox proportional hazard regression with marginal effects, adjusted for comorbidities and injury severity, was conducted to assess the effect of IR intervention for PT compared to BT.
Results: 186,684 patients were identified in the database, 133,074 (71.28%) in the BT group and 53,610 (28.72%) in the PT group. 22,631 (17.01%) in the BT group and 5,036 (9.39%) in the PT group underwent IR intervention. 46,076 (34.63%) patients in the BT group were female, compared to 6,770 (12.63%) in the PT group (p < 0.001). 96,392 (72.43%) in the BT group were White, compared to 19,578 (36.52%) in the PT group (p < 0.001). Mean injury severity score (ISS) for the BT group was 24.15 (SD: 15.09) compared to 18.75 (SD:13.94) in the PT group (p < 0.001).
IR intervention for PT was associated with a 16.67% decrease in risk of mortality compared to IR intervention for BT (HR: 0.83; 95% CI: 0.74-0.93; p=0.002). Average days of survival for non-IR for BT was 260.31 days (SD: 14.5), IR for BT was 201.38 days (SD: 2.62), non-IR for PT was 214.81 (SD: 14.35), and IR for PT was 197.75 days (SD: 5.67)
Conclusions: Based on our survival analysis in a national trauma databank, IR for PT was associated with lower mortality risk compared to the effect of IR for BT. Our retrospective analysis may provide insight in the use of IR for PT.
