Back
Venous Intervention
051 - Ultrasound vs. Fluoroscopy Guidance for Endovascular Arteriovenous Fistula Creation

Subhash Gutti, BA – Medical Student, George Washington University School of Medicine and Health Sciences; Deepak Iyer, BS – Medical Student, George Washington University School of Medicine and Health Sciences; Bohan Liu, MD – Resident Physician, George Washington University Hospital; Hannah Gissel, MD – Resident Physician, George Washington University Hospital; Shawn Sarin, MD, MBA, FSIR – Assistant Professor of Radiology, Interventional Radiology, George Washington University Hospital; Daniel Scher, MD – Assistant Professor of Radiology, Interventional Radiology, George Washington University Hospital
Purpose: Recent technological advancements have allowed for two endovascular approaches to arteriovenous fistula (endoAVF) creation as an alternative to surgical AVF creation for patients with end-stage renal disease and suitable vascular anatomy. While both systems utilize concomitant ulnar or radial arteries and veins, one device uses ultrasound guidance (uAVF) while the other uses fluoroscopic guidance (fAVF). In this study, we aim to compare the technical feasibility and procedural outcomes of endoAVF creation using uAVF or fAVF.
Material and Methods: A systematic review was performed using the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) guidelines to compare the technical aspects and procedural outcomes of uAVF to fAVF.
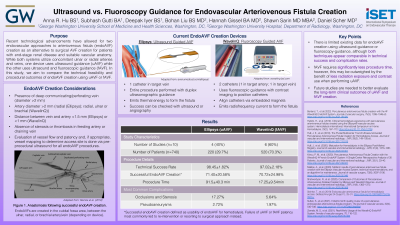
Results: 10 studies totalling 740 patients were included in the final analysis, of which 4 studies evaluated uAVF (Ellipsys; Avenu Medical, San Juan Capistrano, California) and 6 studies evaluated fAVF (WavelinQ; Beckton Dickinson, Franklin Lakes, New Jersey). The technical success rate for uAVF was 98.45±1.82%, while that of fAVF was 97.02±2.18%. Successful endoAVF creation, defined as usability for hemodialysis, for uAVF was 71.40±20.58%, while that of fAVF was 70.72±24.98%. Failure of uAVF or fAVF patency most commonly led to re-intervention or resorting to surgical approach instead. The most significant difference between uAVF and fAVF was procedure time (91.5±40.3 min for uAVF vs 17.25±9.54min for fAVF). While few complications were observed with both devices, the most common serious adverse events noted were occlusions and stenosis (17.27% for uAVF and 5.64% for fAVF) and pseudoaneurysms (2.72% for uAVF and 1.97% for fAVF).
Conclusions: Currently, there is limited existing data for endoAVF creation using ultrasound-guidance or fluoroscopy-guidance, although both techniques appear comparable in technical success and complication rates. fAVF requires significantly less procedure time, however, this may be outweighed by the benefit of less radiation exposure and contrast use when performing uAVF. Future studies are needed to better evaluate the long-term clinical outcomes of uAVF and fAVF creation.
Material and Methods: A systematic review was performed using the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) guidelines to compare the technical aspects and procedural outcomes of uAVF to fAVF.
Results: 10 studies totalling 740 patients were included in the final analysis, of which 4 studies evaluated uAVF (Ellipsys; Avenu Medical, San Juan Capistrano, California) and 6 studies evaluated fAVF (WavelinQ; Beckton Dickinson, Franklin Lakes, New Jersey). The technical success rate for uAVF was 98.45±1.82%, while that of fAVF was 97.02±2.18%. Successful endoAVF creation, defined as usability for hemodialysis, for uAVF was 71.40±20.58%, while that of fAVF was 70.72±24.98%. Failure of uAVF or fAVF patency most commonly led to re-intervention or resorting to surgical approach instead. The most significant difference between uAVF and fAVF was procedure time (91.5±40.3 min for uAVF vs 17.25±9.54min for fAVF). While few complications were observed with both devices, the most common serious adverse events noted were occlusions and stenosis (17.27% for uAVF and 5.64% for fAVF) and pseudoaneurysms (2.72% for uAVF and 1.97% for fAVF).
Conclusions: Currently, there is limited existing data for endoAVF creation using ultrasound-guidance or fluoroscopy-guidance, although both techniques appear comparable in technical success and complication rates. fAVF requires significantly less procedure time, however, this may be outweighed by the benefit of less radiation exposure and contrast use when performing uAVF. Future studies are needed to better evaluate the long-term clinical outcomes of uAVF and fAVF creation.
