Back
Introduction: Obesity, or high body mass index (BMI), is a known risk factor for renal cell carcinoma and predictor of poorer outcomes in general. Our aim is to perform a systematic review and meta-analysis to evaluate the impact of BMI on oncological (primary) and surgical (secondary) outcomes of patients who underwent nephrectomy.
Methods: The review protocol was registered in PROSPERO with ID CRD42021275124. Studies were identified from four electronic databases. Two independent authors conducted the screening and data extraction, while a third resolved discrepancies. Studies which addressed post-nephrectomy oncological and surgical outcomes were included.
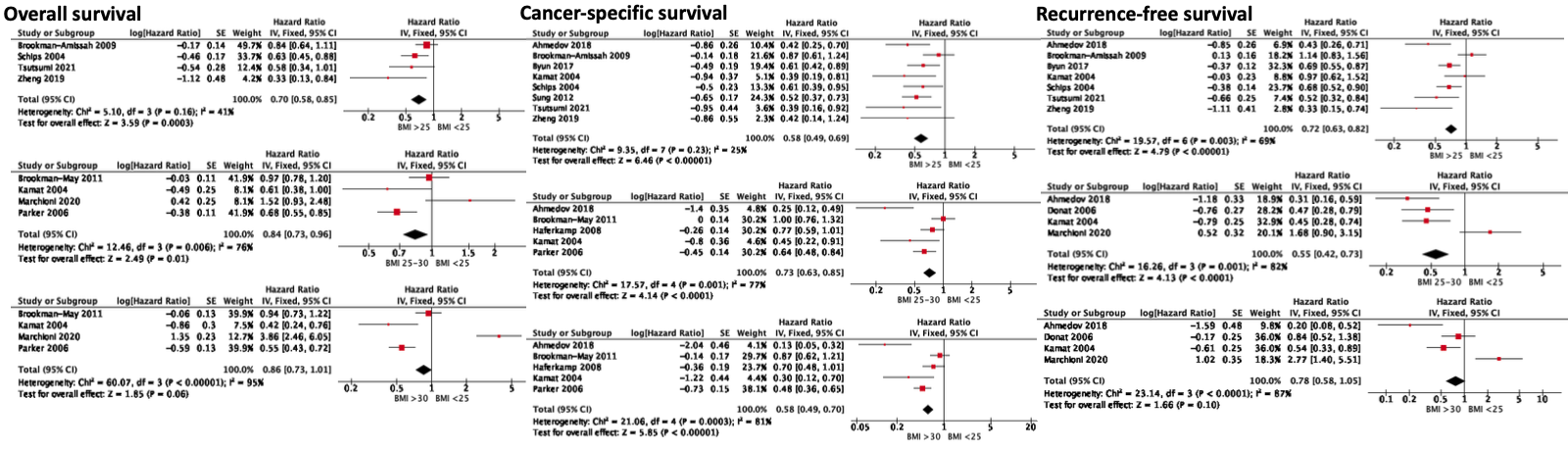
Results: Twenty-three studies consisting 18,546 patients were identified for the final meta-analysis. Regarding oncological outcomes, higher BMI was shown to predict higher overall survival (BMI >25 versus BMI <25: HR 0.70, 95% CI 0.58—0.85, p<0.001; BMI 25-30 versus BMI <25: HR 0.84, 95% CI 0.73—0.96, p=0.01), cancer-specific survival (BMI >25 versus BMI <25: HR 0.58, 95% CI 0.49—0.69, p<0.001; BMI 25-30 versus BMI <25: HR 0.73, 95% CI 0.63—0.85, p<0.001; BMI >30 versus BMI <25: HR 0.58, 95% CI 0.49—0.70, p<0.001) and recurrence-free survival rates (BMI >25 versus BMI <25: HR 0.72, 95% CI 0.63—0.82, p<0.001; BMI 25-30 versus BMI <25: HR 0.55, 95% CI 0.42—0.73, p<0.001). Lower BMI fared better in surgical outcomes such as operation time and warm ischaemic time, although the absolute difference was minimal and unlikely to be clinically significant. There was no difference between groups for length of hospital stay, intra-operative or post-operative complications, blood transfusion requirements, and conversion to open.
Conclusions: Our study suggests that higher BMI is associated with improved long-term oncological survival and similar perioperative outcomes as lower BMI. More research into the underlying biological and physiological mechanisms will enable better understanding of the effect of BMI, beyond mere association, on post-nephrectomy outcomes. SOURCE OF
Funding: NA
Moderated Poster Session
Session: MP47: Kidney Cancer: Localized: Surgical Therapy II
MP47-14: The impact of body mass index (BMI) on oncological and surgical outcomes of patients undergoing nephrectomy: a systematic review and meta-analysis
Saturday, April 29, 2023
3:30 PM – 5:30 PM CST
Location: S504

Edmund Chiong, MD
National University Hospital, Singapore
Poster Presenter(s)
Introduction: Obesity, or high body mass index (BMI), is a known risk factor for renal cell carcinoma and predictor of poorer outcomes in general. Our aim is to perform a systematic review and meta-analysis to evaluate the impact of BMI on oncological (primary) and surgical (secondary) outcomes of patients who underwent nephrectomy.
Methods: The review protocol was registered in PROSPERO with ID CRD42021275124. Studies were identified from four electronic databases. Two independent authors conducted the screening and data extraction, while a third resolved discrepancies. Studies which addressed post-nephrectomy oncological and surgical outcomes were included.
Results: Twenty-three studies consisting 18,546 patients were identified for the final meta-analysis. Regarding oncological outcomes, higher BMI was shown to predict higher overall survival (BMI >25 versus BMI <25: HR 0.70, 95% CI 0.58—0.85, p<0.001; BMI 25-30 versus BMI <25: HR 0.84, 95% CI 0.73—0.96, p=0.01), cancer-specific survival (BMI >25 versus BMI <25: HR 0.58, 95% CI 0.49—0.69, p<0.001; BMI 25-30 versus BMI <25: HR 0.73, 95% CI 0.63—0.85, p<0.001; BMI >30 versus BMI <25: HR 0.58, 95% CI 0.49—0.70, p<0.001) and recurrence-free survival rates (BMI >25 versus BMI <25: HR 0.72, 95% CI 0.63—0.82, p<0.001; BMI 25-30 versus BMI <25: HR 0.55, 95% CI 0.42—0.73, p<0.001). Lower BMI fared better in surgical outcomes such as operation time and warm ischaemic time, although the absolute difference was minimal and unlikely to be clinically significant. There was no difference between groups for length of hospital stay, intra-operative or post-operative complications, blood transfusion requirements, and conversion to open.
Conclusions: Our study suggests that higher BMI is associated with improved long-term oncological survival and similar perioperative outcomes as lower BMI. More research into the underlying biological and physiological mechanisms will enable better understanding of the effect of BMI, beyond mere association, on post-nephrectomy outcomes. SOURCE OF
Funding: NA

