Sedation
434 - Further Evaluations of Pediatric Dental Sedation Airway Intervention Score
- NL
Nadia Latifi, DDS
Pediatric Dental Resident
University at Buffalo/Women and Children’s Hospital of Buffalo, Buffalo, NY
Williamsville, New York, United States - JH
Julie Heard, Pre-Medical Student
University Pediatric Dentistry
- JM
- TT
Tammy Thompson, DDS
University at Buffalo
Buffalo, New York, United States 
Christopher Heard, MD
Anesthesiologist
University at Buffalo, New York
Buffalo, New York, United States
Presenting Author(s)
Co-Author(s)
Program Director(s)
Research Mentor(s)
Purpose: Airway complications are a major concern during Pediatric Dental Sedation. We have previously developed an airway intervention score (Presented AAPD 2021 & 2022) to assess the need for airway support during sedation. The aim of this study is to assess modifications to the components of the score to improve both its interrater reliability and efficacy.
Methods: Following Institutional Review Board authorization, children of 5 to 17 years old who scheduled for oral or intravenous dental sedation procedures were recruited. Modifications included changes in clinical practice, improving logic progression of the score overall and the components of the score. The airway score was independently assessed the operating dentist and the sedation resident or anesthesiologist. We plan to recruit 250 patients.
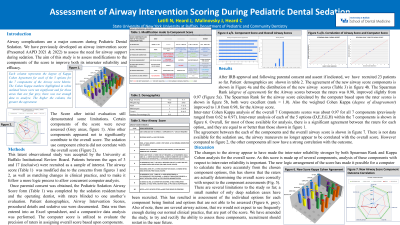
Results: Following parental consent, we have recruited 23 patients so far. Spearman Correlation for Airway scores improved from 0.97 to 0.98. The Weighted Cohen Kappa remained at 0.98 for the Airway score. We also made changes to the airway component matrix table. For the 7 components of the airway score the association with the overall Airway score is presented; Oxygen use and Chin/Jaw had a strong correlation ( > 0.6), only the Sedative use had a poor correlation. The Sedative use was also the only component that was not statistically significant with respect to its correlation with the overall Airway score.
Conclusions: We anticipate that the alterations or correlations to the new airway score table will improve interrater reliability once more data can be analyzed.

.jpg)