Sedation
415 - Evaluation of Deep Sedation Outcomes with respect to Cannabis Use

Jihwan Kim, DDS
Resident
University at Buffalo/John R. Oishei Children's Hospital
University at Buffalo School of Dental Medicine
Buffalo, New York, United States
Amanda Torsney, DDS (she/her/hers)
Pediatric Dentistry Resident
University at Buffalo/Women and Children’s Hospital of Buffalo, Buffalo, NY
University at Buffalo
Buffalo, New York, United States- TV
Timothy Votta, MD, DDS
University Pediatric Dentistry
- JH
Julie Heard, Pre-Medical Student
University Pediatric Dentistry
- JM
- TT
Tammy Thompson, DDS
University at Buffalo
Buffalo, New York, United States 
Christopher Heard, MD
Pediatric Anesthesiologist
Oishei Children’s Hospital
Buffalo, New York, United States
Presenting Author(s)
Co-Author(s)
Program Director(s)
Research Mentor(s)
Purpose: We have noted that there appears to be an increase in the reported use of cannabis in our oral surgery patient population. This can have deleterious effects on the effectiveness and safety of procedural sedation. We plan to use a cannabis use/experience questionnaire to determine cannabis exposure and match the cannabis use patterns with sedation outcomes in young adults for third molar extractions under propofol based deep sedation.
Methods: After IRB approval and with informed consent, adult patients, completed a 5-minute cannabis use questionnaire prior to sedation administration. The patients were categorized into 7 cannabis user groups based on the reported answers in the questionnaire. For analysis, the 7 user groups were sorted into 4 USER categories: non-USER (USER group 0), light-USER (USER groups 1-2), moderate-USER (USER groups 3-4), and heavy-USER (USER groups 5-6). The patient demographics, medical history, sedation use, and outcomes were obtained from the sedation records. Our weight based dosing algorithm was used for the sedation.
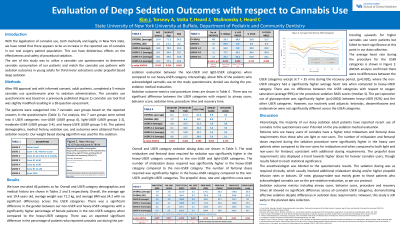
Results: We have recruited 46 patients so far. Overall, the average age was 19.4 years old, average weight was 71.2 kg, and average BMI was 24.2 with no significant differences across the USER categories. There was no significant difference between the USER categories with respect to airway score, behavior score, sedation time, procedure time and recovery time. There was no difference between the USER categories with respect to oxygen saturation (average 99%) or the procedure sedation RASS scores (median 4). The total midazolam and fentanyl dose required for sedation was significantly higher in the heavy-USER category compared to the non-USER and light-USER categories. The number of midazolam doses required was significantly higher in the heavy-USER category compared to the non-USER category. The number of fentanyl doses required was significantly higher in the heavy-USER category compared to the non-USER and light-USER categories. The propofol dose, rate and algorithm curve were trending upwards for higher cannabis use score patients but failed to reach significance at this point in our data collection.
Conclusion: Patients who are heavy users of cannabis have a higher total midazolam and fentanyl dose requirements than those who are light or non-users. The number of midazolam and fentanyl doses required during the sedation procedure were significantly higher in the heavy user patients when compared to the non-users for midazolam and when compared to both light and non-users for fentanyl, consistent with additional dosing requirements. The propofol dose requirements also displayed a trend towards higher doses for heavier cannabis users, though results failed to reach statistical significance. Sedation outcome metrics including airway score, behavior score, procedure and recovery times all showed no significant difference across all cannabis USER categories, demonstrating effective sedation despite differences in sedation dose requirements. However, this study is still early in the planned data collection.

.jpg)