Special Health Care Needs
206 - Clinical Protocol Evaluation of Enamel and Dentin Direct Resin Bonding to Permanent Molars in the Management of Dentinogenesis Imperfecta
- RJ
Ryan Jelicich, DDS (he/him/his)
Dental Fellow
Children’s National Medical Center, Washington, D.C.
Childrens National Hospital
Washington, District of Columbia, United States - ES
Erik Scheifele, DMD
Children's National Hospital
- MC
Mudrika Chhabra, DMD
Program Director
Children’s National Medical Center, Washington, D.C.
Washington, District of Columbia, United States
Presenting Author(s)
Co-Author(s)
Program Director(s)
Purpose:
The purpose of the study is to survey the current restorative/bonding techniques of newly erupted permanent teeth in specialized clinics in the United States to best understand the management of pediatric dental patients who have Dentinogenesis Imperfecta. The study should help identify current clinical practices with the hopes of developing future Best Clinical Practices or Clinical Practice Guidelines for managing patient's with DI.
Methods:
This study will consist of a cross-sectional study implementing an online survey of providers treating patient's with Dentinogenesis Imperfecta. The survey will contain 10 questions utilizing a combination of Likery Scale and standard multiple-choice questions for simplicity in grading and consistency. The study population will include Program Directors at both hospital and academic Pediatric Dentistry Programs in the United States and additional adjunct faculty who manage patients with Dentinogenesis Imperfecta. Approximately 125 individuals will be recruited to complete the study. Participants are to be recruited via email and survey is to be collected via a Google Forms Survey.
Results:
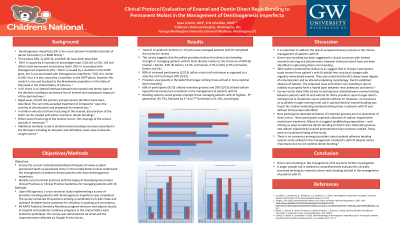
Total of 15 pediatric dentists (n=15) who have managed patients with DI completed the survey for review.
The survey suggests that the polled providers believe that direct resin bonding strength in managing patients with DI most directly relates to the structure of 40% (6) Enamel + Dentin, 33% (5) Dentin, 13,3% (2) Enamel, 6.7% (1) DEJ, 6.7% (1) Enamel, Dentin and CEJ.
80% of surveyed participants (12/15) utilize a total etch technique as opposed to a selective etch technique 20% (3/15).
Providers vary greatly in the belief that longer etching times will aid in more optimal dentin bonding.
60% of participants (9/15) utilized retention grooves and 20% (3/15) utilized sodium hypochlorite enamel pre-treatment in the management of patients with DI.
Bonding systems varied greatly amongst those managing patients with DI highest-- 6th generation (35.7%), followed by 5th and 7th Generation (21.4%), accordingly).
Conclusion:
Direct resin bonding in the management of DI warrants further investigation.
A larger sample size is needed to comprehensively evaluate the clinically practiced techniques related to direct resin bonding utilized in the management of patients with DI.

.jpg)