Back
Practice Innovations
(PI-019) Heel Offloading Posterior Splint for Treatment of Heal Ulcerations

Co-Author(s):
Robin Lenz, DPM, FACFAS
Introduction: Total contact casting is the gold standard for plantar foot ulcers but has been questioned in heel pressure ulcers. Current offloading of heel ulcers is typically removable offloading boots. We describe using a modified posterior splint to offload heel ulcers in non-weight-bearing patients. The posterior splint is readily available and familiar to practitioners, with less of a learning curve than a total contact cast. As part of the dressing, the posterior splint is less likely to be removed, leading to increased compliance. This should translate to improved healing of pressure ulcers.
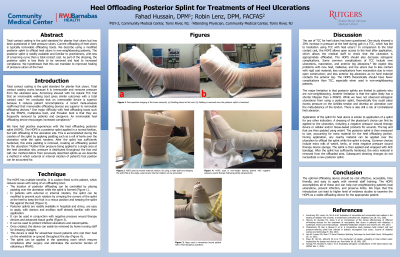
Methods: The application of the splint for heel ulcers is similar to the application of the splint for any other indication. A dressing of the physician's choice can be first applied to the ulceration, including a wound VAC or advanced tissue graft. The leg and foot are then padded using webril. The posterior splint is then measured to size. Any nearby material such as extra rolls of webril or kerlix can be applied over the ulceration while the splint is drying. After the splint has hardened, the extra material is removed. Subsequent dressing changes do not necessitate a new posterior splint.
Results: The HOPS has multiple benefits. It is custom-fitted to the patient, which reduces issues with the sizing of an offloading boot. The location of posterior offloading can be controlled by placing padding over the ulceration while the splint is formed. In patients with external or internal rotation, the splint can be modified to prevent such rotation by crimping the corners of the splint at the heel to keep the foot in a rectus position and keeping the splint flat against the bed. The HOPS is not easily removable and thus removes the issue of compliance.
Discussion: The optimal offloading device should be cost-effective, accessible, time-friendly, and easy to apply with minimal staff training. The HOPS accomplishes all these and can help non-weight-bearing patients heal ulcerations, prevent infection, and preserve limbs. We hope that this introduction can lead to a higher level of evidence studies to examine the HOPS as a viable offloading device for the appropriate patients.
Trademarked Items:
References:
Methods: The application of the splint for heel ulcers is similar to the application of the splint for any other indication. A dressing of the physician's choice can be first applied to the ulceration, including a wound VAC or advanced tissue graft. The leg and foot are then padded using webril. The posterior splint is then measured to size. Any nearby material such as extra rolls of webril or kerlix can be applied over the ulceration while the splint is drying. After the splint has hardened, the extra material is removed. Subsequent dressing changes do not necessitate a new posterior splint.
Results: The HOPS has multiple benefits. It is custom-fitted to the patient, which reduces issues with the sizing of an offloading boot. The location of posterior offloading can be controlled by placing padding over the ulceration while the splint is formed. In patients with external or internal rotation, the splint can be modified to prevent such rotation by crimping the corners of the splint at the heel to keep the foot in a rectus position and keeping the splint flat against the bed. The HOPS is not easily removable and thus removes the issue of compliance.
Discussion: The optimal offloading device should be cost-effective, accessible, time-friendly, and easy to apply with minimal staff training. The HOPS accomplishes all these and can help non-weight-bearing patients heal ulcerations, prevent infection, and preserve limbs. We hope that this introduction can lead to a higher level of evidence studies to examine the HOPS as a viable offloading device for the appropriate patients.
Trademarked Items:
References:

.png)