Category: Respiratory Infections - Bacterial
Poster Session: Respiratory Infections - Bacterial
1466 - Antibiotic utilization reports may reduce prescribing practices for Upper Respiratory Infections

David Augusto Terrero Salcedo
Infectious Disease Fellow
University of Cincinnati
Cincinnati, OhioDisclosure: I do not have any relevant financial / non-financial relationships with any proprietary interests.
- AK
Allison Kelly
MD
US Department of Veteran Affairs
Cincinnati, OhioDisclosure: I do not have any relevant financial / non-financial relationships with any proprietary interests.
- VT
Victoria Tate
PharmD
Cincinnati VA Medical Center
Cincinnati, OhioDisclosure: I do not have any relevant financial / non-financial relationships with any proprietary interests.
Presenting Author(s)
Co-Author(s)
Background: More than 90% of Upper respiratory tract infections (URI) have a viral etiology; nonetheless, these represent the most common reason for ambulatory antibiotic prescription. This translates in higher risk of antibiotic-related adverse events and promotion of antimicrobial resistance.
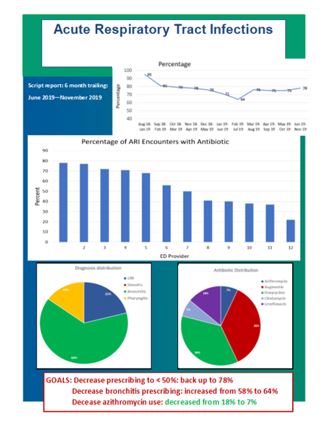
Methods: A prospective single-center intervention surveying and providing individual, face-to-face comparative reports of antibiotic utilization, for any of the 4 diagnostic entities that constitute upper respiratory tract infection (common cold, pharyngitis, acute rhinosinusitis and acute bronchitis), was performed in our Emergency Department. Example of monthly provider reports used which included general and individualized goals.
Results:
A total of 12 health care providers were followed for 12 months. Education, prescribing reports and individual goals were provided. The pre-intervention prescription rate from September to December 2018 averaged 74.75% (SD 20.59, 95% CI 61.6-87.8), with a post-intervention rate of 55.5% from September to December of 2019 (SD 19.20, 95% CI 43.3-67.7) that was statistically significant (p=0.0036). A higher use of antibiotic was observed in physicians when compared to non-physician providers in both pre and post intervention stages (reduction of 16.6% vs 23% after intervention respectively), with no statistical difference between the two groups (CI 95% of -38.82 to 2.395, p=0.0773). A proposed target of 50% or less was observed in 5 of 12 providers (41.6%), and 2 out of 12 (16.7%) had increase in their antibiotic utilization rate.Comparative use of antimicrobials in the pre (September-December 2018) and post (September-December 2019) - intervention periods.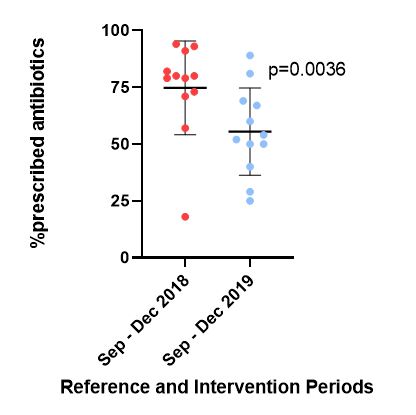 Average individual antimicrobial use rate before and after intervention.
Average individual antimicrobial use rate before and after intervention.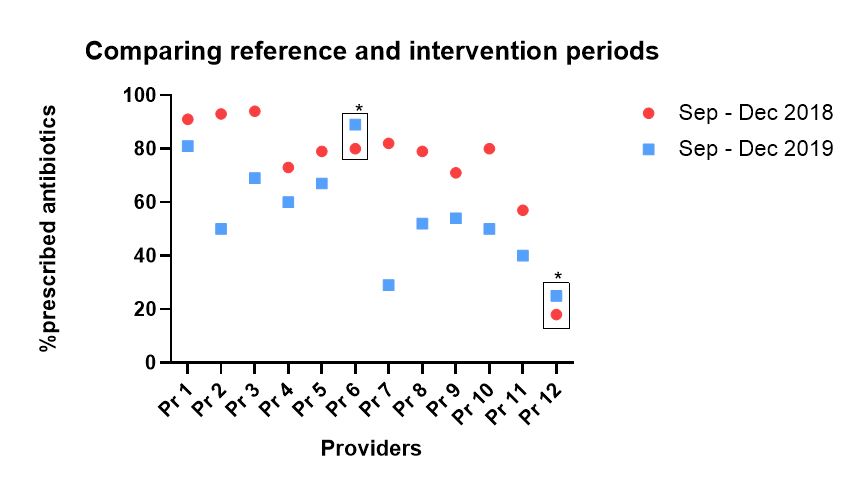
Conclusion: Routine face-to-face utilization reports may constitute an effective approach in reducing antibiotic prescription practices in the Emergency Department, and potentially, in other outpatient healthcare settings.

